Quick Links
Neuro-ophthalmology
Neuro-ophthalmology is a highly specialized branch of eye care that deals with visual problems related to the nervous system. These conditions often originate from issues involving the optic nerve, brain, or eye movement pathways and can affect how we see, interpret, and respond to visual information. Unlike most other eye conditions that arise directly from the eye itself, neuro-ophthalmic disorders stem from neurological dysfunctions and can be complex to diagnose and manage.
Patients with neuro-ophthalmic issues may experience unexplained visual loss, double vision, abnormal eye movements, or even symptoms like headaches and dizziness. Early identification and coordinated care with neurologists, radiologists, and internists are often essential for a proper diagnosis and comprehensive treatment plan.
Read MoreCommon Neuro-Ophthalmic Conditions
Optic Neuritis
Inflammation of the optic nerve often associated with autoimmune diseases like multiple sclerosis. It causes sudden vision loss, eye pain (especially with movement), and color desaturation.
Papilledema
Swelling of the optic disc due to increased intracranial pressure. It may signal serious neurological issues like brain tumors or meningitis and often presents with headache and transient vision loss.
Ischemic Optic Neuropathy
A sudden loss of vision due to poor blood flow to the optic nerve. It may occur in older adults with vascular risk factors and needs prompt intervention.
Cranial Nerve Palsies
Affect movement of one or both eyes due to paralysis of cranial nerves III, IV, or VI. Symptoms include double vision, drooping eyelid (ptosis), and abnormal eye alignment.
Myasthenia Gravis (Ocular Type)
An autoimmune disorder where communication between nerves and muscles breaks down, leading to fluctuating drooping eyelids and double vision.
Thyroid Eye Disease (TED)
Also known as Graves’ orbitopathy, this condition affects the muscles and tissues around the eyes, leading to bulging eyes, double vision, and restricted eye movement.
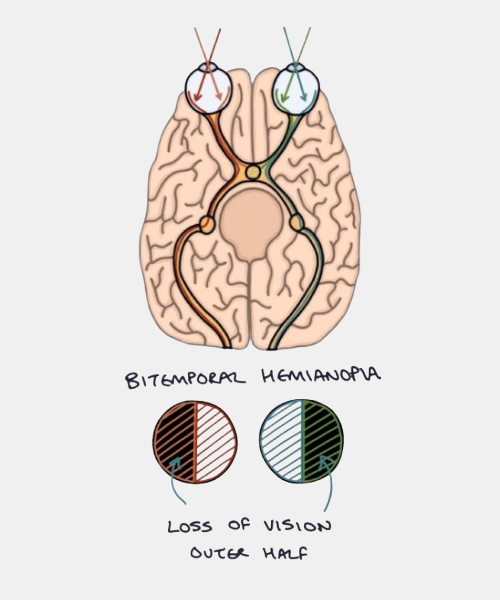
Visual Field Defects
Loss of part of the visual field due to optic nerve damage or lesions in the visual pathway (from the optic nerve to the brain's occipital lobe). Often associated with stroke, tumors, or trauma.
Symptoms of Neuro-Ophthalmic Disorders
Sudden or Progressive Vision Loss
Loss of vision in one or both eyes can occur abruptly or gradually. This may indicate optic nerve inflammation, ischemia, or compression, and requires immediate assessment.
Eye Pain with Movement
Pain when moving the eyes, especially during upward or sideward gaze, is often associated with optic neuritis or orbital inflammation.
Drooping Eyelids (Ptosis) or Eyelid Twitching
Weakness or fatigue of the eyelid muscles can signal a neuromuscular disorder like myasthenia gravis or nerve palsy affecting eyelid function.
Blurred or Double Vision (Diplopia)
Misalignment of the eyes due to nerve or muscle involvement can cause overlapping or ghost images. Diplopia may worsen with fatigue and varies with gaze direction.
Loss of Peripheral (Side) Vision
Tunnel vision or blind spots (scotomas) may result from damage to the optic nerve or visual pathway lesions in the brain, such as from stroke or tumors.
Unequal Pupil Size or Abnormal Light Response
Anisocoria or sluggish pupil reaction can be signs of optic nerve disease, third nerve palsy, or increased intracranial pressure.
Visual Hallucinations or Flashing Lights
Seeing flickering lights, patterns, or shapes without external stimuli may indicate retinal or cortical disturbances, including occipital lobe pathology.
Headache Associated with Visual Changes
Persistent or severe headaches with vision problems may point to increased intracranial pressure, papilledema, or inflammatory neurological diseases.
Diagnostic Tools and Technology
Visual Field Testing
Assesses peripheral vision and identifies patterns suggestive of neurological lesions.
Optical Coherence Tomography (OCT)
Provides detailed imaging of the optic nerve and retinal layers.
MRI/CT Imaging
Brain and orbit scans to detect tumors, inflammation, demyelination, or vascular anomalies.
Fundus Photography
For monitoring optic disc swelling or pallor over time.
Electrophysiology (VEP/ERG)
Measures electrical responses in the visual system to detect nerve conduction abnormalities.
Blood Tests and Autoimmune Panels
Help identify systemic causes like lupus, vasculitis, or thyroid dysfunction.
Management and Treatment Options
Steroid Therapy
Intravenous or oral corticosteroids are commonly used for conditions such as optic neuritis and thyroid eye disease. They help reduce inflammation and prevent permanent nerve damage when started early.
Immunosuppressants
Autoimmune disorders like myasthenia gravis or neuromyelitis optica may require long-term immunomodulatory drugs to control disease progression and protect visual function.
Surgical Intervention
When structural compression, tumors, or severe thyroid-related eye disease are involved, surgery may be necessary. Procedures could include orbital decompression, muscle realignment, or tumor excision, often done in collaboration with neurosurgery or ENT specialists.
Botox Injections
Botulinum toxin is used in cases of eyelid spasms (blepharospasm), nystagmus, or to temporarily relieve certain types of double vision due to muscle imbalance.
Prism Glasses or Eye Patching
For managing diplopia (double vision), prisms in glasses help realign images for comfortable vision. In some cases, alternate eye patching may reduce symptoms temporarily while underlying conditions are treated.
Neurological Referral
Since many neuro-ophthalmic issues stem from systemic or central nervous system disorders, co-management with neurologists, endocrinologists, or internal medicine specialists is often essential for comprehensive diagnosis and treatment.
FAQ's
How is neuro-ophthalmology different from general ophthalmology?
Neuro-ophthalmology deals with visual problems caused by neurological diseases rather than problems limited to the eyes alone.
Can vision loss from optic neuritis be reversed?
In many cases, vision improves partially or fully over time, especially with early steroid treatment.
Is double vision always a sign of nerve palsy?
Not always. Double vision can arise from muscle imbalance, neurological disorders, or even thyroid eye disease. Accurate diagnosis is key.
What if I have a headache with vision loss?
This could be a sign of increased intracranial pressure or other serious conditions and requires urgent evaluation.
Can neuro-ophthalmic conditions be permanently cured?
Some conditions like optic neuropathies may cause irreversible damage, but many others can be treated effectively if caught early.